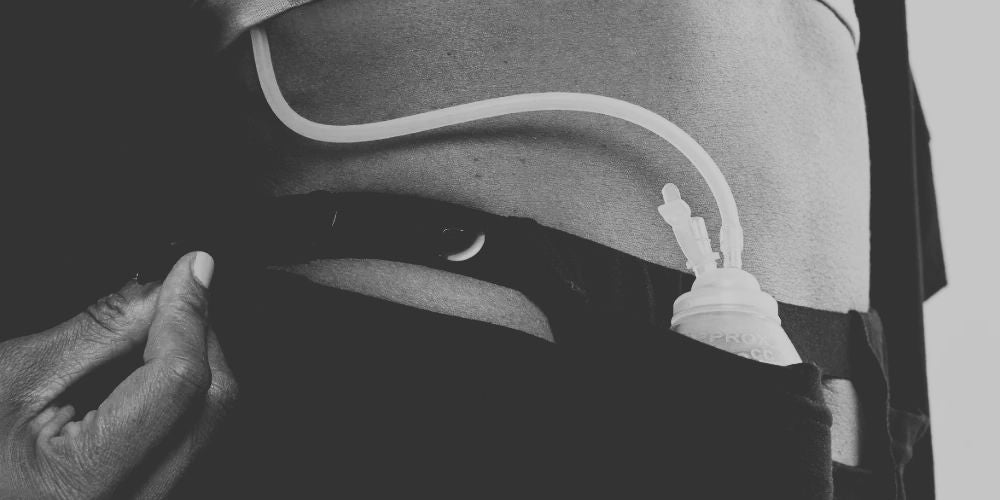
Mastectomy Drains and Care: What You Should Know
What is the #1 complaint post-mastectomy? The drains! We know all about those dreaded drains here at AnaOno, and in this article we hope to take a little of the “dread” out of drains.
Many major surgeries optimize the use of drains after a procedure, especially one that is directed to the removal of tissue and other body masses. The purpose of the drains is to collect the added fluids built up by the body in its effort to heal to ensure a smoother healing process. Especially following a bilateral mastectomy or unilateral mastectomy you can almost always expect to have anywhere between two and six drains depending on the amount of tissue removed, your body type, and the choice of reconstruction surgery. Not to worry, though; below are our top tips on how to manage drains post-mastectomy.

What Is The Purpose Of A Mastectomy Drain?
The purpose of post-mastectomy drains is to aid in the healing processes after the removal of breast tissue is completed. “The body often builds up fluid and can cause discomfort and delay healing if not drained,” says VeryWellHealth in an article explaining the science behind mastectomy drains and why they are needed to help heal.
Many surgeries require drains, but they are especially common in mastectomy surgeries. This is due to the amount of tissue that is required to be removed to treat the cancerous tumor or after undergoing a preventative mastectomy. Some reconstruction surgery revisions may also require drains. If undergoing a revision surgery where the implant is changing from under the muscle (UTM) to over the muscle (OTM), drains may also be required to manage any additional fluid build up post-op.
Caring For Your Drain
Breast surgeons and plastic surgeons will give you a very extensive list of how to care for the drains. One task post-surgery will be managing the drainage output by how much fluid is building up in the bulbs. We won’t lie, this process can be a bit stomach twisting. If you are not someone that handles blood well, we recommend you prepare your caregiver to help you manage through this process.
Keeping your drains in place is part of the battle, and that is why we recommend easy loungewear garments like our Miena Recovery Robe and Abby Lounge pant to help. Both comfy pieces in our Recovery Collection have pockets to help you manage and hold drains in place. What’s great with the drain belt is that it is easily detachable, machine washable, and super comfy.

Each Miena Robe with drain management system includes a super helpful and easy tracker chart so you can keep our output organized and tracked for your follow up appointments.
Need an additional tracker? Download it here and print it out to keep it by your bed for marking your measurements and take with you on your follow-up appointments.
Living With Your Drain
Managing your drains through everyday activities may feel cumbersome, but we have some helpful tips to get you through.
- Showering: We recommend finding a shower shirt or shower pouch to help manage drains during bath time. This will help keep your drains protected and out of harm's way so you can focus on scrubbing all the right places after your mastectomy surgery.
-
Sleeping: Managing drains while you doze in and out during recovery could feel stressful. Make sure the drains are secured in a pocketed hoodie or other carrier in order to have them managed while you get some much needed zzz’s.
- Dressing: Having bulbs hanging from your body is not something you are likely used to, so dangling drains can get in the way. A simple and super affordable option is to get a lanyard and clip the drains around your neck while you get dressed to keep them safely secured and in front of your body. You could also consider getting an additional detachable drain management belt to secure those drains in place while you slowly and safely get dressed for the day.
- Driving: As long as you have your drains secured in a pocket or pouch, riding in a car to and from your doctors appointments should be well managed, however, please check with your doctor for driving restrictions. With limited range of motion, pain in your chest, and other challenges following a mastectomy driving a vehicle is NOT recommended.
- Getting around: Drains can stay in from 2-4 weeks post-mastectomy, and trust us, by the end you may be feeling like removing these things yourself, but you absolutely can not! As you begin to move more and more, you may find the drains more cumbersome than when you were relaxing and recovering. Not to worry, though; you will learn how to protect the drains and keep them out of your way. Remember, though: the more you relax and recover, the better off you are. Doing too much too soon can increase drainage output and keep the drains in longer. Be sure to check with your physicians to understand your physical restrictions during recovery.

Common Mastectomy Drain Problems
Common drain problems following a mastectomy could include risk of infection, issues with your incision site, or pressure loss in the drain.
If you feel something isn’t right and you think you have a problem with your drain after your mastectomy, call your doctor immediately. Complications happen and there is always some level of risk in any surgery or procedure. The biggest risk could be infection and it is something to take very seriously.
When Should You Contact Your Doctor?
If you are experiencing an increase in your drainage output instead of a decrease, call your doctor. If you are experiencing heat, rash, or burning at your incision site of the drainage tube, call your doctor. If you have a loss of vacuum pressure in the drain, call your doctor.
There is never a moment during recovery where you should feel too proud to call or text your doctor a photo of a concern you are having, even if it is for peace of mind.
For more information, check out “10 Reasons To Call The Doctor’s Office About Wound Healing with JP Drains” by The Breast Institute of Houston. These top tips can direct you to when it is time to call your doctor after a mastectomy with drains.
How Are Mastectomy Drains Removed?
As a part of the recovery and follow-up process post-mastectomy, your doctor will make the final call of when it is time to remove the drains. Typically, they will base this decision off of the amount of fluid that is being produced day after day.
Be sure to ask your physician what the optimal output is, so that you can alert the staff to get the drains removed. You may want them out sooner than they can, so just be patient. We get it. This part isn’t easy, but you just got through a mastectomy surgery and you are strong!
Want More Info On How To Manage Your Drains Post-Mastectomy?
We love the article “What to Expect” on BreastCancer.org and all their other supporting content. Vetted by medical professionals and written by an expert staff, there are tons and tons of helpful articles throughout the site to help you navigate a cancer diagnosis and all that comes with it. There is also a forum for other breast cancer patients and survivors where you can ask questions and get answers.

Frequently Asked Questions
How long do you have drains after mastectomy?
Post-Mastectomy drains can be used for 2-4 weeks post-op. Be sure to check with your doctor on the estimated time your drains may be in following surgery. Some drains are removed within days, others after a few weeks.
How many drains will I have after mastectomy?
How many drains post-mastectomy will depend on your surgery decisions and body type. If having a unilateral mastectomy, most patients can expect 1-2 drains. A bilateral mastectomy can yield the need of 2-6 drains depending on the amount of tissue removed and body type.
What is the fluid that drains after a mastectomy?
The fluid that drains from the body after a mastectomy is called serous fluid. Serous fluid is the result of raw tissue and will slow its development inside the body when the tissue begins growing back together. Serous fluid is a natural part of the healing process and wants to come out and that is why drains are used to aid in that process.
Does it hurt to have drains removed after breast surgery?
Everyone’s experience will be different, however the tubes inserted into the surgery site are often very small. With the expert removal done by your plastic surgeon and care providers, it is not often painful to have the drains removed following a mastectomy surgery. If you experience any pain around the incision site, we strongly recommend reaching out to your physician to discuss.
DISCLAIMER: This website does not provide medical advice. The content on this page is strictly for informational purposes only, and is not meant to be used as professional medical advice or treatment. Always consult a licensed physician with any questions or concerns regarding drain management and care, and never delay seeking medical attention because of something you have read on this website.